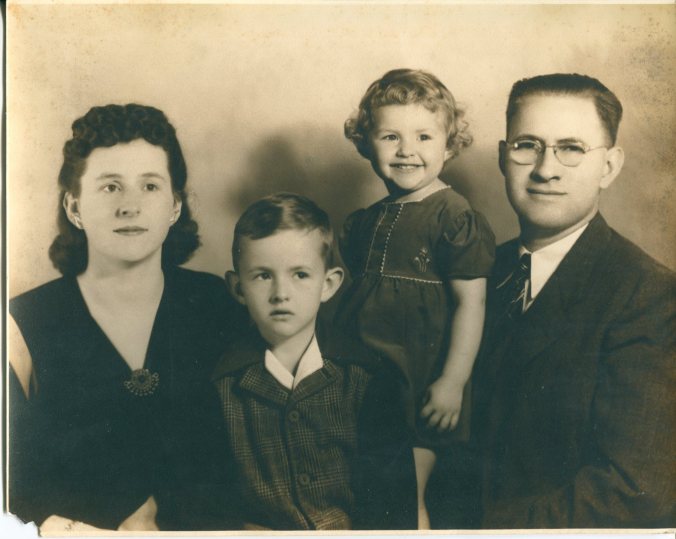Diagnosis stories are powerful teaching tools that help people learn to recognize the symptoms of type 1 diabetes. For the person diagnosed with type 1 diabetes, a diagnosis is the day his or her life changes and goes forward. Semisweet is sharing “Richard’s Diagnosis Story” in his own words. Richard has been living with type 1 diabetes for over 70 years. In 2006 he joined the diabetes online community, where people were fascinated to hear Richard’s story of living with T1D in the 1940s and beyond. In 2010, Richard published his autobiography, “Beating The Odds: 64 Years Of Diabetes Health.”
Richard, diagnosed at age 6, September 1945
I was born in 1939, in Roanoke, VA, and I had several illnesses before my fifth birthday: three different kinds of measles and my tonsils removed. When I was five I had chicken pox and mumps, and while recovering I began showing the classic symptoms of diabetes— excessive peeing and drinking so much water. My parents took me to three different doctors, but they did not recognize my symptoms, so there was no diagnosis. I lost my appetite, and refused to eat. I just wanted to drink.
One doctor prescribed a tonic that was supposed to restore my appetite. I still remember the bad taste and tall glass bottle filled with dark brown liquid. It was like the snake oil medicine that we have read about from the past. The tonic did not help at all. It probably made my condition worse because it contained sugar. By the time we saw a fourth doctor I was very weak, and had lost a lot of weight. My ribs were very noticeable when my shirt was removed. The fourth doctor recognized my symptoms, and took a blood sample in his office. The sample was sent to a lab, and we waited a few days before returning to his office for the results.
His office was on the second floor of a building on Main Street in Salem, VA, and I struggled to slowly walk up the long flight of stairs. My father was carrying my three year old sister, but I was too big to be carried. In the doctor’s office, my mother and I sat in chairs while my father stood behind us, still holding my sister. I do not remember the doctor’s face, or his words, but I’ve never forgotten my mother’s pale and frightened face. In September 1945, a few days after my sixth birthday, we were told that I had sugar diabetes. I was hospitalized the next day, and don’t remember much about the stay, except for the injections and the blood that was collected. Insulin, taken from pigs or cows caused me to gradually regain my appetite, and I stopped losing weight. By the time I was home, I looked like a human being again, and my strength was very much improved.
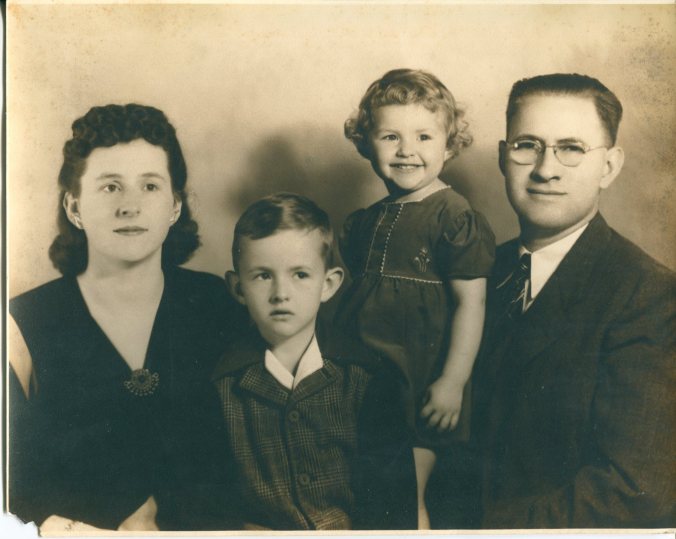
Richard and his family a few months after his diagnosis
While in the hospital, I was treated by Dr. Davis and he became the doctor for my whole family. I saw him every six months, and he took blood samples, testing them in his office lab while I waited. My blood sugar was always high, but I don’t recall him ever mentioning numbers. We were not concerned though because we did not know about the complications that might occur with my eyes, kidneys, and other body parts. One shot per day, one urine test, large portions of food, and no worries. Ignorance was bliss.
There were no meters for testing blood sugar at home until the 1980s, almost forty years after my diagnosis. We tested my urine at home, every morning, but the procedure for doing that was very awkward. The first thing I did each morning was to pee in a cup. Some Benedict’s solution was placed in a large test tube, and several drops of urine were added. The test tube was placed upright in a container of water on our stove. When the water had boiled a while, the test tube was removed, and the color of the solution was observed. The original color of the Benedict’s solution was blue. If the solution containing the urine was blue, after boiling, then there was no sugar present in the urine. If sugar was present in my urine, then there would be colors: green, yellow, orange, brick red, or brown. Green showed a low amount of sugar, brown showed very high sugar.

testing blood sugar with Benedict’s solution
It was nice that there was only one injection each day before breakfast, but there were no fast and slow acting insulins, so control of my blood sugar levels was not good at all. The animal insulin was a 24 hour insulin, so the morning urine test result determined the dosage, but urine tests do not approximate blood sugar well. The glass syringe and metal needles were kept in alcohol, and sterilized with boiling water on the stove once each week. We had our own well, and the water contained limestone deposits. After boiling, there was a white film on the needles and syringe, so we had to use a whetstone to remove the deposits. The limestone frequently clogged the insides of the needles, so we had to push a small wire through the needles to unclog them. If the deposit was not removed it was difficult to push the needle into my skin. The needles were almost three quarters of an inch in length. I was supposed to push the needle into the muscle on top of my legs, or on my arms. My father gave me my injections until I was ten.
During the night I would sometimes have hypos. Some of those hypos became seizures. I would thrash around during my sleep, my teeth clinched, my muscles would become drawn, and I was almost unconscious. Mother poured small amounts of the sugar water they kept nearby on my lips, until I had enough in my mouth to partially awaken me. Then I drank the liquid more freely. I was always drenched with sweat, and very weak after a seizure. My body was sore the next day and the sugar water caused my urine test to show high the next morning. I continued to have seizures for many years, but they occurred less frequently when I was older. There was never any effort made to call an ambulance. Perhaps it was because the nearest hospital was at least 10-15 miles from our house, and I doubt that the paramedics in the ambulance had glucagon injections. Home care was probably the best solution. I think my mother saved my life many times during the years I lived at home.
Dr. Davis told us that I should not eat sugar, but no other instructions about an appropriate diet were given, so we didn’t know about carbohydrates. We lived on our little ten acre farm, and we had cows, chickens, pigs, and a horse. There was a very big garden, and an orchard. We bought very little food at the grocery store, so processed food was rarely part of my diet. Our own milk, eggs, vegetables, and fruit were readily available. We had meat from the chickens and pigs. Mother canned food each summer and fall. I helped my father with the farm work, and I was very hungry, so I ate big portions at every meal. I ate all the same food that my parents and sister ate, except items containing sugar. Mother used saccharin to sweeten the pies, cookies and cakes that she made for me. I ate lots of bread, potatoes, and other things that were not good for me, but we thought all foods were okay, if they did not contain sugar.
My parents did the best they could for me during my childhood and Dr. Davis gave no instructions that helped. We did not know there could be potential problems, and I led a rather normal day to day existence. There were no health problems with my diabetes throughout my childhood, despite my very irregular blood sugars. I have often wondered why I did not have DKA back then. Was something protecting me? All the fast acting carbs I ate each day (without correction boluses like I take now) must have kept my blood sugar very high. I’m sure my parents were devastated by my diabetes, and not knowing how to care for me. My parents raised me in much the same way that they were raised in their mountain homes. They were raised on farms, and they loved that kind of living.
When I talk to parents of T1D children diagnosed today, I advise them to join online diabetes support groups for parents. Children with Diabetes, created by Jeffrey Hitchcock, and the many parents’ support groups on Facebook are very good sources of advice and information for parents. Getting support from experienced parents can help so much! There are books that are available, but I think the online community is best. Having T1D children meet other children in their communities is a very good idea. Diabetes camps in the summertime are an excellent idea. Attending the Friends For Life conference in Orlando, FL is another source that I have seen work so well with children who are type 1.

Richard at 76, having lived with T1D for 70 years
If you’d like learn more about Richard’s life with type 1 diabetes, then check out this video interview where Richard shares his experiences with Daniele Hargenrader. Richard was also interviewed about living with T1D for over 7 decades on Diabetes Mine. Richard will also be a speaker at the 2016 FFL conference in Orlando, FL. You can follow Richard on Twitter @Richardvau157.





 Alexis Johansen teaches in the 4 and 5 year old room at the University of Northern Iowa Child Development Center with her Bachelors in Early Childhood Education. She recently just finished up her third year teaching. Alexis lives in Cedar Falls, Iowa with her newly married husband and her adorable dog that loves to cuddle! When she isn’t at school with her kiddos, she enjoys reading, running, and being crafty at home.
Alexis Johansen teaches in the 4 and 5 year old room at the University of Northern Iowa Child Development Center with her Bachelors in Early Childhood Education. She recently just finished up her third year teaching. Alexis lives in Cedar Falls, Iowa with her newly married husband and her adorable dog that loves to cuddle! When she isn’t at school with her kiddos, she enjoys reading, running, and being crafty at home.